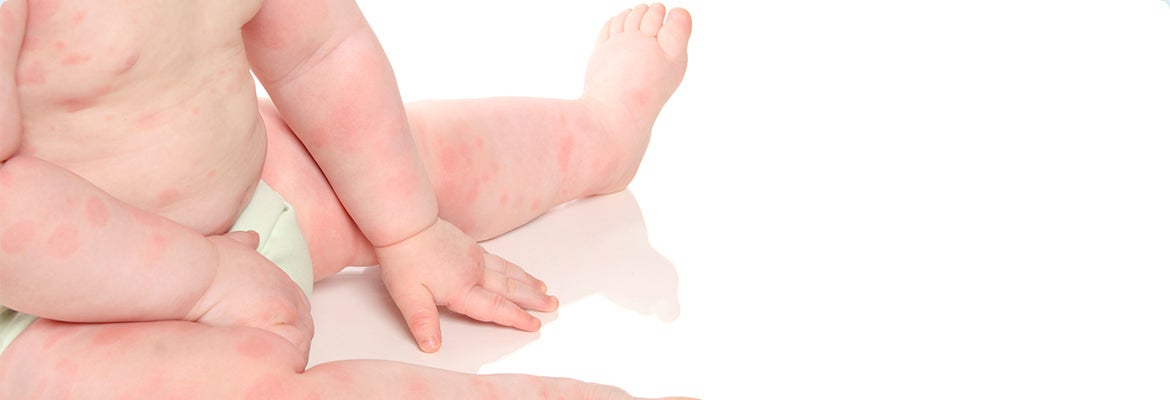
Baby Allergies and Intolerances
Statistics show that food allergies and intolerances are rising steeply, including in young babies. While the causes are complex and linked to several factors, the phenomenon itself is now well-identified: the organism comes into contact with a substance it does not recognise (or no longer recognises as safe) and activates its defence system in order to eliminate the intruder. While there are many different symptoms, the solution is to eliminate the ingredient from your baby's diet and reintroduce it slowly at a later date. This is best done under the supervision of a dietitian and paediatric allergist.
Here are some answers to key questions you may have on the subject.
Does breastfeeding help to prevent food allergies?
Generally speaking, breastfeeding may reduce the risk of food allergies.
In high-risk families with a history of allergies (father, mother, etc.), particularly allergies to proteins found in cow's milk, breastfeeding is strongly recommended. Ideally, your baby should be exclusively breastfed in early life. From the point of view of the immune system, breastfeeding makes your baby more resistant. The digestive system also matures more effectively. It is beneficial for solid foods to be introduced gradually while your baby is still being breast fed.
What symptoms do these allergies produce?
Depending on the food responsible, symptoms to look out for can include vomiting, diarrhoea, stomach pain, hives, slight swelling of the lips and tongue, eczema, asthma and recurrent ear, nose and throat infections, not forgetting possible disruption to the child's growth rate.
What are the main allergenic foods?
From the introduction of solids until three years of age the four main allergenic foods are: eggs, gluten, peanuts and cow's milk proteins.
Eggs
Egg allergy is the most common type of food allergy in Australian children. If your child is diagnosed with an egg allergy, note that many food products are manufactured using ingredients containing eggs - read the label and list of ingredients carefully. A dietitian can help teach you the best way to read the food label. Always introduce cooked egg to your baby.
Gluten
Gluten is a protein found in cereals such as rye, oats, wheat (including bread wheat, spelt and kamut) and barley. As soon as a gluten allergy is diagnosed, all products derived from these cereals must be eliminated from the diet. Until a diagnosis is made it is recommended gluten be introduced from six months even if there is a family history of allergy. Doing so, with the added protection of breastfeeding, may decrease the chances of developing Coeliac Disease and this is an area of active research.
Peanuts
Like eggs and gluten, peanuts are present in many industrial food products not designed for children. It is up to you to read the label in order to detect the slightest presence and avoid them if your baby has a confirmed allergy, otherwise, you may introduce small tastes of natural peanut butter during solids introduction in the first year.
Cow's milk proteins
Allergy to cow’s milk proteins is common, particularly in young infants.
Other categories of potentially allergenic ingredients:
- Dried fruit;
- Other Tree nuts (hazelnuts, pistachio nuts, almonds, walnuts);
- Tropical fruits (kiwi fruits, mangos),
- Seeds (poppy, sesame);
- Modified proteins (soya protein, surimi);
- Protein-based food additives (α-amylase, carmine, casein, vegetable starch);
- Legumes (broad beans, beans, peas, chick peas);
- Berries (strawberries, raspberries);
- The latex group (bananas, avocados, chestnuts).
What you should know:
- Always cook fruit and vegetables thoroughly (before reducing them to a purée or compote) as cooking can reduce their allergenic properties;
- Introduce new foods one at a time - preferably in the morning so you are alert to any adverse reactions over the course of the day;
- If possible, continue to breastfeed during the introduction of solid foods.
Who can diagnose an allergy?
In the first instance, your GP or paediatrician may prescribe a blood test. It is then recommended that you consult an allergist. You can even find specialised infant allergists.
Can allergies be cured?
No medical cure currently exists for food allergies. However it is possible that your baby will outgrow their allergy so your doctor may challenge your child at specific time points to check this, under medical supervision.
Cow's Milk Allergy or Intolerance
Cow's milk may be the cause of either an allergy to the proteins (casein or whey) found in cow's milk which provokes a defensive reaction by the immune system or an intolerance to the sugar in milk (lactose), often resulting from an insufficient secretion of lactase, the enzyme which breaks down lactose, in the intestine.
The number of cases of allergies to cow's milk proteins has doubled in the past ten years (there are many causes and the list is still vague according to specialists). “In Australia and New Zealand around 2 per cent (1 in 50) babies are allergic to cow's milk and dairy products. Although most children outgrow cow's milk allergy by the age of 4 years, persistent cow's milk allergy may sometimes occur. However, ongoing symptoms in adults are very rare.” Australasian Society of Immunology and Allergy (ASCIA).
It is not easy to recognise this type of allergy or intolerance as the signs vary and may be confused with other conditions.
Indications of an allergy to cow's milk proteins:
- Skin: hives, eczema, redness or paleness in the face, oedema (swelling);
- Digestive: regurgitation, vomiting, constipation, chronic diarrhoea (in newborns), stomach pain (in young children);
- Respiratory: wheezy cough, asthma, difficulty breathing.
The outcome if diagnosed
If your baby is seen by a paediatric allergist, an extensively hydrolysed-protein formula will often be prescribed. This substitute for cow's milk is designed for young infants (not to be confused with a HA formula). This special milk is no less rich than your baby's previous milk formula and will contribute just as effectively to his growth. Your doctor will determine the most appropriate feeding plan for your infant.
Indications of lactose intolerance include:
- acute and irritable diarrhoea that can be frothy;
- bloating and stomach cramps;
- excessive wind;
- nappy rash;
- reflux
In order to confirm the suspicions of your healthcare professional, your child may be asked to undergo full allergy testing with a specialist. Tests are often inaccurate and elimination and retrial of suspected foods may be the better option.
There is a history of allergies in my family. Is this a factor?
A parent or sibling may be allergic to cow's milk without the new baby inheriting the same allergy. That said, a higher level of food allergies have been observed in families with a history of allergy and intolerances. If you have a family history of allergies you should let your health professional know as this may help them determine the best way to possibly prevent allergies occurring in your baby.
What about soy milk?
The Australasian Society of Immunology and Allergy (ASCIA) advise that there is no benefit of giving soy formula if a young infant has a diagnosed cow milk protein allergy.
What foods to give
Although an allergy to cow's milk will complicate the manner in which you feed your baby, your allergist and regular healthcare professional will be able to advise and help you throughout his nutritional development. Remember your baby may outgrow the problem.